Healthcare professionals are becoming increasingly concerned that the long-term effects experienced by those COVID-19 patients who were hospitalised, may be underestimated.
This is evidenced by a new study published in the medical journal The Lancet, that showed that six months after becoming ill, 1,733 people experienced lingering problems including fatigue, anxiety, depression, insomnia and diminished lung capacity.
Of the 2,469 COVID-19 patients discharged, from the Jin Yin-tan Hospital in Wuhan, China, only 1,733 were eligible for the study that found that more than three-quarters of them had at least one persistent symptom six months later. To date, this is the largest study with the longest follow-up.
The methodology used in-person evaluations of individuals who had been admitted to the hospital for a median of 14 days between 7 Jan to 29 May 2020. All patients were interviewed using a series of questionnaires in order to evaluate the symptoms and related quality of life.
They also underwent physical examinations, a six-minute walking test and a blood test. About 350 patients were tested for lung function and had chest CT scans and ultrasounds. The median age of the eligible patients was 57.
The researchers found that the most common single issue (63%) was ongoing fatigue and muscle weakness. Over 25% experienced sleeping difficulties and 23% also reported anxiety and depression (a symptom that was found to be more common in women).
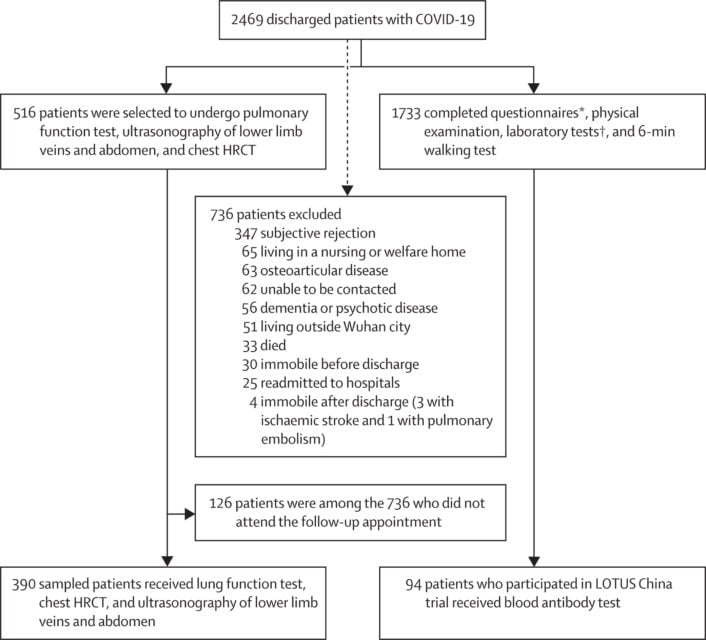
Flow chart of patients with COVID-19 discharged from Jin Yin-tan Hospital between Jan 7, and May 29, 2020: Source: Chaolin Huang et al. 2021
Those patients who were more severely ill during their time in hospital often displayed impaired lung function and abnormalities were detected during the chest imaging, indicating possible organ damage.
Additionally, the study also revealed that some people who were hospitalised had normal kidney function when they were admitted but displayed diminished kidney function later on.
The authors acknowledge that the study may not be the first to address the issue of long-term persistent symptoms, also known as ‘Long COVID’ but they believe that most studies published to date appear to have either used patient samples that were too small or too short a timeframe, as many studies were carried out over a maximum period of three months.
There are also important aspects that the study doesn’t delve into, such as the patients’ cognitive or neurological functions; neither does it report whether any patients suffered from anxiety or depression before the onset of COVID-19. It is also limited to being a single-centred study of solely Chinese patients.
Nonetheless, even though the study may not be considered comprehensive, it is of importance.
To begin with, it is one of the first publications that really describes with some degree of detail longer-term outcomes among a relatively large group of people. Secondly, it forms part of a growing body of evidence that confirms what many individuals have long been reporting: chronic, often debilitating health issues that are still hard to define and as yet not well understood.
As the pandemic unfolded across the globe, patients joined Facebook groups, Twitter feeds, and other online support groups to share their stories of the symptoms that they were experiencing post-COVID, bringing visibility to an issue that has come to be called ‘Long COVID’.
Many people described wide-ranging symptoms that included cognitive issues, known as “brain fog”, memory or attention problems, shortness of breath, a racing heart, nausea, diarrhoea, intermittent spiking fevers and much more.
Many more researchers are now launching follow-up studies of people who have been infected with COVID-19. A number of these will focus on damage to specific organs or systems while others plan to track a range of effects.
In the United Kingdom, the Post-Hospitalisation COVID-19 Study (PHOSP-COVID) aims to follow 10,000 patients for a year, analysing clinical factors such as blood tests and scans, and collecting data on biomarkers. A similar study by the University of California, San Francisco, on long-term coronavirus symptoms will follow hundreds of patients for up to two years.
Understanding the long-lasting effects of COVID-19 on patients, even those who experienced mild symptoms, remains crucial to planning the healthcare system response in countries all over the world.
Doctors and healthcare professionals have warned that without a proper understanding of the long term effects, these could turn out to be a bigger public health problem than the deaths caused by the pandemic – deaths which were not simply the result of COVID-19 but also due to delayed diagnoses and interventions as a result of the emergency.












